When we think of ketones or ketogenic diets, most people think of brain health, seizure control, sports performance, or as a diet therapy for cancer management, but the heart thrives on fatty acids and ketones. Probably because ketones are used by the mitochondria to generate ATP and mitochondrial density accounts for around one third of the cardiac myocyte. Under normal conditions, the heart generates nearly all of its energy from fat (>85%), and that changes in a failing vs nonfailing state (see in Science)
Ketones and the heart
The liver makes ketones in response to low glucose availability and the suppression of insulin when we fast, follow a ketogenic diet, and after prolonged exercise. Beta-hydroxybutyrate (BHB) is the body’s primary circulating ketone body, and the ketone body of interest and focus of this blog. We can also ingest exogenous, or supplemental, BHB (e.g., ketone salts), which get delivered preferably to tissues with high oxidative demands, like the heart! A very interesting phenomenon is the increase in blood beta-hydroxybutyrate (BHB) during heart failure and it appears that the failing heart will switch to burning ketones as an alternative fuel. Heart failure is a condition where the heart can no longer support its energy demands to do its job of pumping blood. It’s been suggested that supplying ketones during heart failure can overcome the heart’s energetic crisis by preserving energy flux and improving hydraulic efficiency. In dogs, it was shown that BHB infusion prevented the expected decrease in oxygen consumption by the heart and preserved heart function when heart failure was induced. There are other lines of evidence that suggest the failing heart will turn to ketones as a way to optimize metabolic efficiency. However, just like the brain, the heart burns ketones in proportion to what’s in circulation, suggesting that blood ketone levels determine ketone metabolism in the heart and that supplemental ketones could enhance the heart’s energy production.
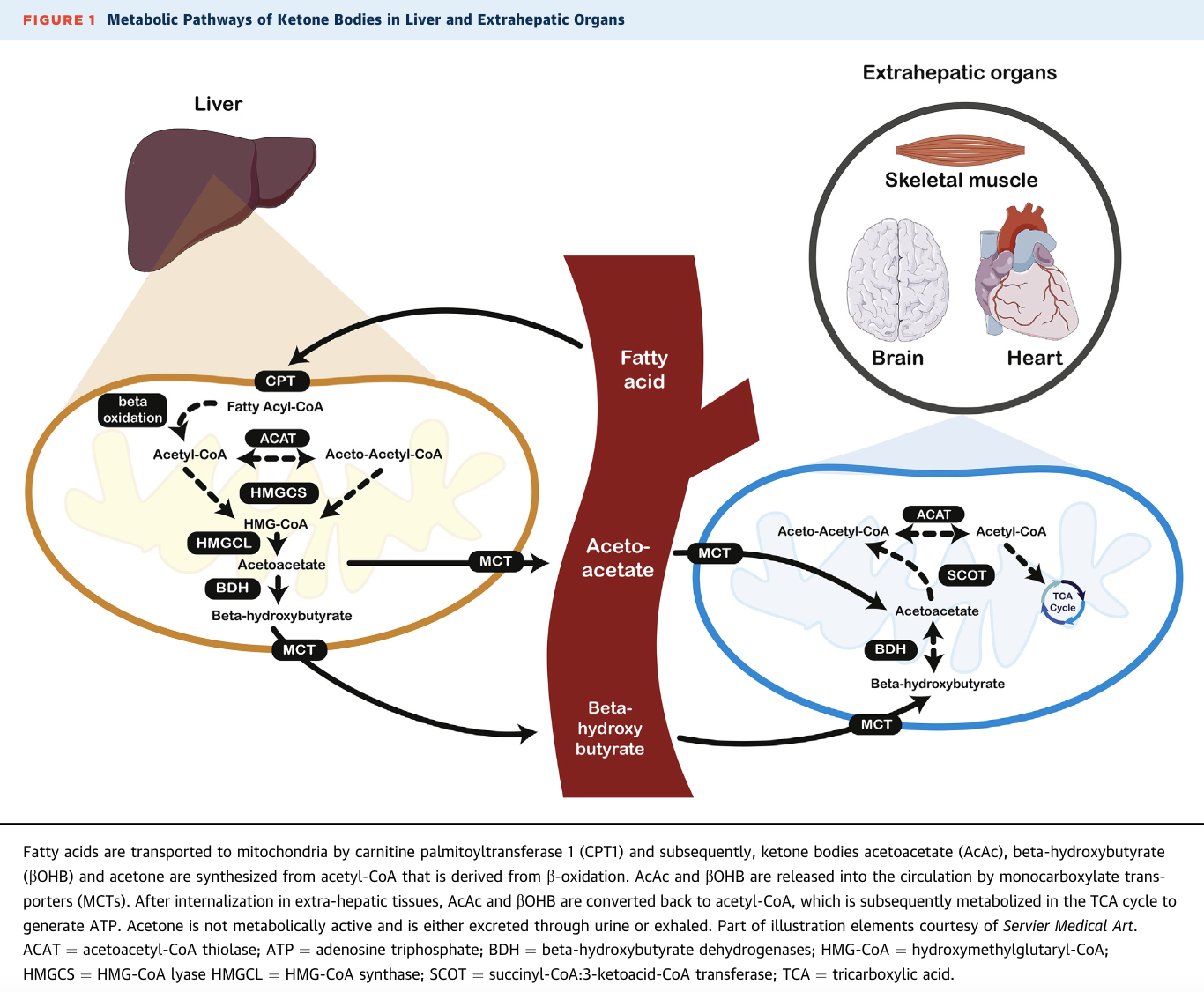
Source: Yurista et al., 2021
Ketones serve other heart-supportive roles beyond simply supplying the heart with energy. For example, in a mouse model over-expressing ketone metabolizing enzymes, increased ketone (BHB) oxidation by the heart was associated with decreased oxidative damage (enhanced SOD, MT2, CAT, and Foxo3a expression and lower ROS) and protection against heart failure under conditions that would otherwise promote damage. This finding is not unique to this study, as BHB has been shown by others to reduce cellular oxidative stress through these mechanisms in addition to increased expression of genes that protect against oxidative stress through epigenetic changes. Infusing BHB in mice has also been shown to reduce mitochondrial stress in the heart after being exposed to ischemia and reperfusion (injury to the heart). In addition to oxidative stress wreaking havoc on the heart, inflammation also contributes to cardiovascular disease. An emerging area of research is investigating BHB’s anti-inflammatory potential through its inhibitory actions on the NLRP3 inflammasome and subsequent reductions in the release of pro-inflammatory molecules such as IL-18, and IL-beta. While the evidence is limited, one way BHB may benefit cardiovascular health is by suppressing systemic inflammation (hsCRP), which would help to preserve metabolic health and blood flow dynamics.
Critical to heart health is of course endothelial function. The endothelium is a thin (single) layer of cells that line our heart and blood vessels and controls blood pressure and flow, in addition to playing important roles in immune regulation, clotting, among others. Importantly, the vascular endothelium produces and releases nitric oxide (NO) which causes vasodilation to increase blood flow. There is some preliminary evidence from animal models that the BHB-precursor, 1,3-butanediol, and ketogenic diet increase the enzyme responsible for endothelial-NO production. In humans, BHB-infusion increases vasodilation and blood flow to the heart by up to 40%!
Ketogenic Diets
Raising blood levels of BHB with supplements is a different physiological state than following a diet low enough in carbohydrates (and to some degree, protein) that induces ketogenesis. Due to the high fat content of a ketogenic diet, it often gets a bad rap when it comes to heart health. Unfortunately, the message of “high fats diets cause CVD” is often applied to ketogenic and low carb diets, but this oversimplification is taken out of context. Typically, the concern with a high-fat ketogenic diet is increased LDL-cholesterol. We addressed this topic in a previous blog and direct you to that for more information. Additionally, there are ways to manipulate the types of fats you are eating to change blood lipids all while sustaining ketosis, suggesting that not all high-fat diets are the same. It is critical to consider that excess body fat directly increases cardiovascular risk factors, including dyslipidemia, insulin resistance, sleep apnea, as well as practically all other metabolic disorders. A well-formulated ketogenic diet can be an excellent method for producing a calorie deficit, losing body fat and improving metabolic health, and thereby lowering the risk of heart disease.
Ketogenic diets, as well as ketone supplements, are also a means of achieving glycemic control. Keeping blood sugar levels in a health range (70-120mg/dL) is ideal for vascular health as frequent blood sugar spikes and chronically elevated blood sugar can be detrimental to the heart and endothelium by increasing advanced glycation endproducts (AGEs), oxidative stress, and inflammation.
Summary
- The heart burns ketones during an energetic crisis (e.g., heart failure)
- You can increase blood ketones with supplements and ketogenic diets
- The signaling effects of BHB may benefit cardiovascular health by supporting mitochondrial function, reducing oxidative stress, lowering inflammation, and improving blood flow which would apply to both exogenous ketones and ketogenic diets
- Ketogenic diets are a method for improving body composition and glycemic control, both of which lower your risk for heart disease.
Written by: Kristi Storoschuk
Edited by: Dr. Dominic D`Agostino
