Managing blood sugar doesn’t only apply to diabetics, but rather the population as a whole. Frequent blood glucose fluctuations can be quite dangerous. In particular, high blood glucose can be very damaging and promotes the onset and progression of many diseases. Various factors alter glucose control, such as age, exercise, diet, health status, and even stress. Human studies have shown that chronically elevated blood glucose can trigger inflammation and oxidative stress, known contributors to various conditions.
Our team has a particular interest in seizure disorders, where inflammation can provoke seizure activity, which in turn promotes further inflammation; an ugly vicious cycle. There are several studies showing an association between high blood glucose levels and seizure frequency, suggesting that hyperglycemia is playing a role in seizure activity. In diabetes, a disease typically associated with poor glycemic control, hyperglycemia consistently contributes to worse long-term outcomes, in addition to promoting inflammation and oxidative stress. Unfortunately, current strategies used for glycemic control are relatively ineffective, are bound to side effects, and/or are unsustainable. If high blood glucose levels persist over time, serious damage can ensue. This includes conditions, such as insulin resistance, impaired insulin secretion, macro- and microvascular complications, increased production of reactive oxygen species (ROS) which contributes to oxidative stress, and inflammation.
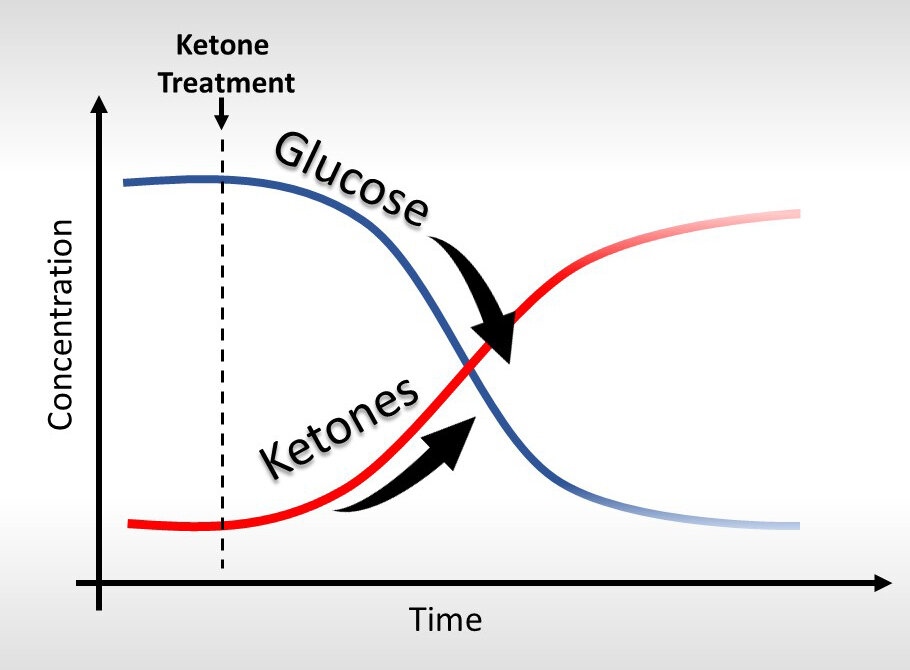
The ketogenic diet is a very effective way to prevent postprandial glucose spikes and improve glycemic control. The restrictive nature of the diet, however, can be difficult for patients to stick to, and maintaining therapeutic ketosis with diet alone can be challenging. For those that find the diet unsustainable, exogenous ketones may be very helpful, and in our recent publication we show their glucose lowering effects, independent of dietary restriction.
We measured how effective exogenous ketones were at lowering blood glucose in rodents under different conditions.
Because glucose regulation changes with age, we tested against different ages.
Because glucose regulation changes with exercise, we tested in rested and post-exercise states.
Because glucose regulation differs between healthy and diseased states, we tested in a non-pathological model and two pathological models (epilepsy and GLUT1 deficiency syndrome).
Animals were fed either standard rodent chow (SD), ketogenic rodent food (KD), or SD + ketone supplementation, in different lengths of administration: acute (1 administration), sub-chronic (7-days), and chronic (10-weeks).
The results demonstrated that exogenous ketones and the ketogenic diet lower blood glucose in short-term and long-term administration. Age, length of administration, type of ketone supplement, rested or post-exercise, and pathological states influenced the degree of glucose control.
What is the real-world relevance?
There are countless conditions that would benefit from glycemic control, diabetes and epilepsy are just two examples. Various neurological disorders, cancers, and many other conditions are linked to glucose control on some capacity. High blood glucose can even hinder recovery from surgery or traumatic injury. In this case, glycemic control can be extremely useful in promoting faster recovery in addition to preventing complications. In the critically ill, better glucose control has also been associated with improved outcomes.
In diabetics, high blood glucose can produce glucose toxicity which is the primary cause of most diabetic vascular complications. Glycemic control has been shown to significantly reduce the risk of diabetic complications. The KD is largely known for its traditional use in epilepsy, but in actuality it was prescribed for diabetes before the advent of insulin, and as of recently it is resurfacing as a therapy for both type-1 and type-2 diabetes. Improving glycemic control with a diet, such as the ketogenic diet, or by use of ketone supplementation, can be extremely advantageous as it is non-invasive, safe, and comes with very little side-effects.
In summary
The ketogenic diet and ketone supplements have the ability to lower blood glucose levels, but the effects differ depending on type of ketone supplement, duration of treatment administration, whether in rested and post-exercise states, age, and disease pathology. Exogenous ketones are a method of reducing blood glucose levels, while also elevating blood ketone levels which is relevant to conditions known to benefit from therapeutic ketosis.
The mechanisms are still to be elucidated, and whether these benefits will translate to humans. It is speculated that the large dose of exogenous ketones could produce a small release of insulin of which would facilitate the removal of glucose from the blood stream and thereby lower blood glucose. Although, in type-1 diabetic children, BHB infusion caused a significant drop in blood glucose, which would suggest that endogenous insulin secretion is not playing a role. Other speculations are that ketones promote better insulin sensitivity and therefore better glucose removal from the blood. More research is needed to verify how exogenous ketones are producing this glucose lowering effect.
Based on these results, exogenous ketones have the potential to be highly therapeutic due to their induction of ketosis and reduction in blood glucose levels.
[youtube=://www.youtube.com/watch?v=Y7UGaW80870&w=854&h=480]
Written by: Kristi Storoschuk; Edited by: Dr. Dominic DAgostino, Dr. Csilla Ari Dagostino
